 No abnormal enhancement could be seen more proximally in the expected location of the cervical plexus or upper cervical spinal nerves. This structure ended at the posterior border of the sternocleidomastoid muscle and was consistent with an enlarged anterior branch and distal main trunk of the great auricular nerve. Both MR imaging and CT showed an enhancing, cylindrical structure that extended inferiorly from the parotid gland, coursing along the lateral aspect of the sternocleidomastoid muscle, and corresponding to the cord-like lesion palpated clinically ( Fig 2). There was no radiologic evidence of deep tumor extension into the substance of the parotid gland or perineural spread along the main trunk of the facial nerve. Both techniques revealed an irregular cutaneous and subcutaneous mass overlying the inferior aspect of the right parotid gland ( Fig 2). There was no cervical adenopathy.ĬT and MR imaging were performed. Additional physical findings included a complete right facial paralysis and anesthesia over the mid- and lower parotid region, in the distribution of the anterior branch of the great auricular nerve. Extending inferiorly and posteriorly from this mass was an approximately 4-cm cord-like structure, which was firm, non-tender, and superficial to the right sternocleidomastoid muscle. A physical examination revealed a well-healed scar in the anterior cheek and a 3.5 × 4-cm mass overlying the inferior aspect of the right parotid gland, just above the mandibular angle. Three years earlier, he had undergone resection of a poorly differentiated squamous cell carcinoma of the right cheek. More distally, the GAN should be lateral to the sternocleidomastoid muscle, with diverging, superiorly oriented routes for the anterior and posterior branches.Ī 70-year-old man presented at our institution with an enlarging mass overlying the right parotid gland and an 8-month history of progressive right facial paralysis. To our knowledge, the GAN has not been described in the cross-sectional imaging literature however, based on the anatomy, the expected course of the GAN would be deep to the sternocleidomastoid muscle for the more proximal aspect of the nerve. The posterior branch communicates with the auricular branch of the vagus nerve and also with the posterior auricular branch of the facial nerve (1). 
The GAN communicates with several cranial nerves in the following manner: the anterior branch sends a small twig (or several small twigs) into the substance of the parotid gland and connects to the facial nerve (1). The posterior branch supplies the skin over the mastoid process and lower external ear, and the anterior branch supplies the skin overlying the parotid gland and lower preauricular region. It then courses superiorly, dividing into anterior and posterior branches. The GAN leaves the cervical plexus at the posterior border of the sternocleidomastoid muscle (Erb's point) and courses anteriorly over the lateral surface of this muscle. 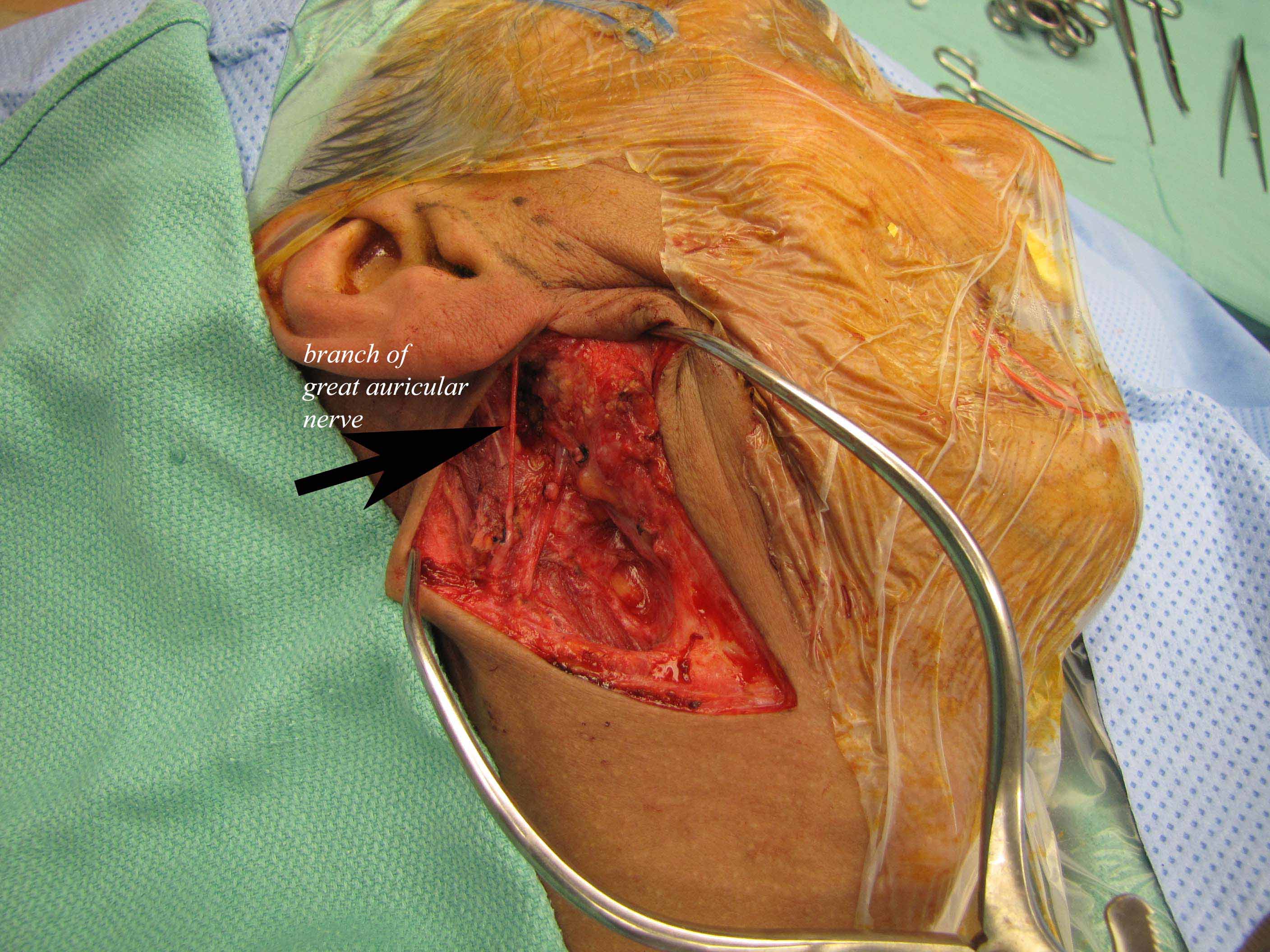
Another well-known deep branch of the cervical plexus is the phrenic nerve (1). One such deep branch is the nervus descendens cervicalis or inferior root of the ansa cervicalis, which forms a loop in conjunction with the hypoglossal nerve and innervates the sternohyoid, sternothyroid, and inferior belly of the omohyoid muscles (1). There are also numerous muscular branches of the cervical plexus that innervate deep muscular structures of the neck (1). The cervical plexus gives off multiple superficial cutaneous branches in addition to the GAN, including the lesser occipital nerve, which innervates the postauricular region, the transverse cutaneous nerve, which innervates the upper anterior neck, and the supraclavicular nerves (1) ( Fig 1). The plexus is anterolateral to the levator scapulae and medial scalene muscles and deep to the sternocleidomastoid muscle (1). The cervical plexus is a complex structure formed by the ventral primary divisions of the first four cervical nerves (1). The GAN is a superficial branch of the cervical plexus, contributed to by fibers from the C2 and C3 spinal nerves (1) ( Fig 1). 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
